Early
Indicators of Atherosclerosis in People with HIV Are Linked to Inflammation,
Improve with Antiretroviral Therapy
 |
 |
 |
 |
 |
 |
 |
| SUMMARY:
Several studies presented at the 17th Conference on Retroviruses
and Opportunistic Infections (CROI
2010) last month in San Francisco looked at atherosclerosis
and its precursors in people
with HIV. Elevated levels of inflammation biomarkers and
indicators of stepped-up T-cell activation were associated
with thickening of artery walls, reduced dilating ability,
and greater artery stiffness. Effective antiretroviral
therapy (ART), however, appeared to slow atherosclerosis
progression. |
|
 |
 |
 |
 |
 |
 |
 |
By
Liz Highleyman
A growing body of evidence indicates that inflammation is associated
with development of non-AIDS conditions such as cardiovascular disease
in people with HIV.
 Atherosclerosis
("hardening of the arteries") is a progressive inflammatory
process in which artery walls thicken and lose their elasticity as they
fill up with plaques made up of accumulated lipids, immune cells, calcium,
and scar tissue fibers. Over time, this leads to impaired blood flow,
which can ultimately result in a heart attack or stroke.
Atherosclerosis
("hardening of the arteries") is a progressive inflammatory
process in which artery walls thicken and lose their elasticity as they
fill up with plaques made up of accumulated lipids, immune cells, calcium,
and scar tissue fibers. Over time, this leads to impaired blood flow,
which can ultimately result in a heart attack or stroke.
Carotid Artery Thickening
A research
group at the University of California San Francisco (UCSF) including
Steven Deeks, Priscilla Hsue, and Peter Hunt have extensively studied
links between inflammation, immune activation, and cardiovascular risk
factors. They presented multiple studies at CROI.
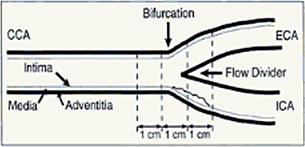 In
an oral presentation (abstract 125), Hsue reported that people with
HIV experience more rapid progression of atherosclerosis than uninfected
individuals, especially as measured in a specific part of the carotid
artery known as the bifurcation region.
In
an oral presentation (abstract 125), Hsue reported that people with
HIV experience more rapid progression of atherosclerosis than uninfected
individuals, especially as measured in a specific part of the carotid
artery known as the bifurcation region.
Intima-media
thickness (IMT), a commonly used early indicator of atherosclerosis,
refers to thickness of the inner layers of the artery wall, where plaques
accumulate. IMT is typically measured using ultrasound in the carotid
arteries in the neck, but results can vary depending on whether a measurement
is taken: in the main artery before it divides, in 1 of its 2 branches
(the internal and external carotid), or at the bifurcation or "fork"
where they split.
Lipids
and other material collect more readily at the bifurcation due to changes
in blood flow dynamics, and therefore it may be more susceptible to
inflammation and show thickening sooner. However, the bifurcation region
(sometimes referred to as the carotid bulb) is harder to measure, so
researchers more often look at other sites.
The
study included 263 HIV positive participants in the SCOPE cohort at
San Francisco General Hospital; most (72%) were on antiretroviral therapy,
47% had suppressed viral load, the median current CD4 cell count was
433 cells/mm3, and the median nadir (lowest-ever) level was 150 cells/mm3.
In addition, the investigators looked at 22 participants from a cohort
of "elite controllers" who are able to maintain undetectable
viral load without ART. There were also 40 HIV negative control subjects.
HIV positive participants had lower LDL (bad) cholesterol at baseline,
but higher levels of triglycerides and the inflammation biomarker high-sensitivity
C-reactive protein (CRP) compared with HIV negative control subjects.
They were also more likely to smoke (68% vs 53%) and had more than twice
the prevalence of high blood pressure, diabetes, and prior heart disease
or strokes, but these differences did not reach statistical significance.
Results
 |
At
baseline, IMT was greater among HIV positive people than HIV negative
individuals, both overall (0.86 vs 0.71 mm) and in each carotid
region. |
 |
After
a median 2 years of follow-up, overall IMT progression was significantly
more rapid in HIV positive group (0.046 vs 0.012 per year). |
 |
The
difference remained significant after adjusting for traditional
cardiovascular risk factors such as smoking. |
 |
Among
HIV positive participants, IMT progression was most evident in the
bifurcation region, followed by the internal carotid and then the
common carotid. |
 |
The
difference in progression between HIV positive and HIV negative
people depended on measurement site: |
| |
 |
Largest
difference in the bifurcation region (0.074 vs 0.013 mm/year,
a significant difference); |
 |
Smaller
but still significant difference in the internal carotid (0.046
mm/year vs none); |
 |
Not
a statistically significant difference in the common carotid
(0.074 vs 0.013 mm/year). |
|
 |
Among
people on suppressive ART and elite controllers, IMT progression
was significantly greater only in the bifurcation region. |
 |
CRP
levels were more closely correlated with IMT progression in the
bifurcation region. |
 |
After
adjusting for traditional risk factors and HIV status, CRP was independently
associated with IMT progression in the bifurcation region. |
 |
However,
traditional cardiovascular risk factors were more predictive in
other carotid regions. |
Based on these findings, the researchers concluded, "HIV-related
inflammation contributes to increased risk of atherosclerosis in the
setting of HIV." They recommended that, "future studies of
sub-clinical atherosclerosis in HIV-infected individuals should focus
on the bifurcation region as a site of marked disease predilection."
Flow-mediated Dilation
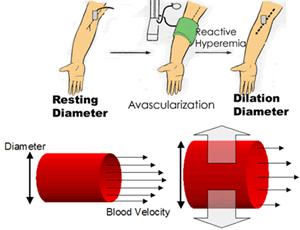 In
a related poster presentation (abstract 708), Hsue and colleagues
looked at another indicator of atherosclerosis progression, flow-mediated
dilation. This technique assesses the function of the endothelial lining
of arteries by measuring how much an artery (typically the brachial
artery in the upper arm) expands in response to changes in blood flow.
In
a related poster presentation (abstract 708), Hsue and colleagues
looked at another indicator of atherosclerosis progression, flow-mediated
dilation. This technique assesses the function of the endothelial lining
of arteries by measuring how much an artery (typically the brachial
artery in the upper arm) expands in response to changes in blood flow.
This study included 139 HIV positive people from the same SCOPE cohort
who had suppressed viral load on ART, as well as 32 HIV negative control
subjects. About half were smokers and about 40% had high blood pressure.
Results
 |
People with HIV had significantly lower -- that is, worse -- endothelium-dependent
flow-mediated dilation compared with uninfected people (4.1% vs
5.2%). |
 |
This
finding remained significant after adjusting for traditional cardiovascular
risk factors. |
 |
Use
of abacavir (Ziagen,
also in the Epzicom
and Trizivir
coformulations) was associated with impaired flow-mediated dilation. |
 |
Protease
inhibitor exposure and overall duration of ART, however, were not
significant predictors of impaired dilation. |
 |
CD4
count was also not significantly linked to impaired flow-mediated
dilation. |
 |
HIV
positive people on ART had a higher median CRP level than HIV negative
individuals. |
 |
CRP
was independently associated with HIV infection after adjusting
for traditional cardiovascular risk factors. |
 |
In
the HIV positive group, higher CRP was a stronger predictor of impaired
flow-mediated dilation than older age, but the opposite was true
for HIV negative people. |
In
this study the investigators concluded, "CRP -- a measure of inflammation
-- was more predictive of impaired endothelial function than traditional
risk factors in this population."
"These
findings suggest that even patients doing well on combination antiretroviral
therapy (as defined by viral load) may be at increased risk for cardiovascular
disease, and that chronic inflammation in the setting of treated HIV
disease likely contributes to this increased risk," they continued.
"Our findings also argue for an independent role of direct drug
toxicity in driving early cardiovascular disease."
T-Cell
Activation and Senescence
Robert Kaplan, along with members of the UCSF team and others (abstract
709) looked at the relationship between carotid IMT and carotid
distensibility (ability to expand) and immune activation in HIV positive
and at-risk HIV women from the Women's Interagency HIV Study (WIHS)
cohort.
The
study included 28 HIV positive women on ART with undetectable viral
load, 46 HIV positive women on ART but with detectable virus, 41 untreated
HIV positive women, and 43 HIV negative women.
T-cell status was determined according to the proportion of T-cells
carrying the CD38+ and HLA-DR+ immune activation markers or the CD57+
and/or CD28- senescence markers. Senescence refers to exhaust of a cell's
ability to proliferate.
Results
 |
CD4
and CD8 T-cell activation was significantly greater among HIV positive
women (of all treatment or response statuses) compared with HIV
negative women. |
 |
Women
on ART with suppressed HIV had significantly lower T-cell activation
than either treated but detectable or untreated HIV positive women. |
 |
However,
even after a median 6 years on ART, T-cell activation did not fall
to the level of the HIV negative women. |
 |
Greater
T-cell activation was associated with lower CD4 cell counts. |
 |
Among
HIV positive women, increased levels of CD4 and CD8 T-cell activation
and senescence markers were independently associated with reduced
carotid distensibility. |
 |
Greater
CD4 and CD8 T-cell activation were associated with carotid lesions
(defined as > 1.5mm carotid IMT) as measured in the right common
carotid artery, internal carotid artery, and carotid bifurcation. |
 |
In
a multivariate analysis adjusting for age and ART status, T-cell
status was an independently predicted higher risk of IMT lesions: |
| |
 |
CD4
T-cell activation: hazard ratio (HR) 1.6, or 60% increased
risk; |
 |
CD8
T-cell activation: HR 2.0, or twice the risk; |
 |
CD8
T-cell senescence: HR 1.9. |
|
 |
Among
HIV negative women, however, there was no observed association between
CD4 or CD8 T-cell status and carotid IMT or distensibility. |
"Among
HIV-infected women, T-cell activation was associated with markers of
sub-clinical carotid artery disease after adjustment for multiple confounders,"
the investigators summarized. "These associations of T-cell activation
and senescence with carotid artery parameters were not observed in a
population of HIV-uninfected controls who were studied using identical
methods and who had comparable cardiovascular risk factor profiles."
"Collectively,
these observations are consistent with a model in which untreated
HIV infection results in immune activation, accelerated immunologic
aging and the emergence of a population of potentially dysfunctional
immunosenescent T-Cells," they concluded. "Antiretroviral
therapy-mediated suppression of HIV replication may only partially reverse
or prevent this process. The presence of a large population of activated
and/or senescent T-cells may be causally associated with premature onset
of cardiovascular disease."
ART and Atherosclerosis
Progression
Jason
Baker and fellow investigators with the Centers for Disease Control
and Prevention's SUN Study (abstract 126) evaluated changes in
carotid IMT and their relationship with ART.
This observational
cohort included HIV positive people in four U.S. cities enrolled during
the modern ART era (2004-2006). Most (78%) were men and the median age
was 42 years. Overall, the group was at low risk for progression to
AIDS; 78% were on ART (about evenly divided between NNRTIs and protease
inhibitors), 71% had a viral load below 400 copies/mL, and the median
CD4 cell count was near normal at 481 cells/mm3 (though the nadir was
about 200 cells/mm3).
Many had traditional cardiovascular risk factors, but overall they were
considered at relatively low risk for cardiovascular disease. About
40% were smokers and about 30% had high blood pressure or metabolic
syndrome. Total and LDL cholesterol levels were generally within recommended
ranges. The median Framingham Risk Score was also low at 2, but 30%
had a score of 5 or higher.
The researchers
used ultrasound to measure IMT in the common carotid artery at study
entry and 2 years later. They then conducted an analysis to determine
factors associated with carotid artery thickening.
Results
 |
Over
2 years of follow-up, the overall median common carotid IMT increased
from 0.710 mm at baseline to 0.720 mm (a median increase of +0.013
mm). |
 |
The
largest proportion of patients, however, showed no change. |
 |
Participants
with consistently suppressed viral load at all study visits showed
a significantly smaller IMT increase than those with 1 measurements
above 400 copies/mL (+0.011 vs +0.019 mm). |
 |
NNRTI
use was associated with a significantly smaller IMT increase compared
with protease inhibitors (+0.009 vs +0.016 mm). |
 |
However,
there was not a significant difference between patients who took
abacavir and those who used tenofovir
(Viread, also in the Truvada
and Atripla coformulations)
(+0.015 vs +0.013 mm). |
 |
After
adjusting for traditional cardiovascular risk factors, the following
factors predicted smaller increases in caroid IMT (all statistically
significant): |
 |
 |
Baseline
viral load suppression (difference of -0.010 mm); |
 |
Persistent
viral suppression during follow-up (difference of -0.014 mm); |
 |
ART
use at baseline (difference of 0.009 mm). |
|
 |
Older
age and being overweight were also independently associated with
larger IMT increases: |
| |
 |
Each
additional 10 years of age increased carotid IMT by a further
0.005 mm. |
 |
Body
mass index > 25 increased IMT by 0.013 mm. |
|
 |
In
this study, however, the high-sensitivity CRP as not a significant
predictor of increased carotid IMT. |
"Maintaining
a suppressed HIV viral load decreased progression of sub-clinical atherosclerosis
(carotid IMT)," the investigators concluded. "Factors related
to both HIV infection and the type of antiretroviral therapy independently
associate with the rate of carotid IMT progression."
Early ART and Arterial
Stiffness
Finally, Jennifer Ho and colleagues from the UCSF team (abstract
707) looked at whether earlier initiation of HIV therapy -- above
the 350 cells/mm3 threshold in effect at the time of the study -- might
reduce cardiovascular risk.
This analysis included men on ART with undetectable plasma HIV RNA chosen
from the SCOPE cohort (who start ART during chronic infection) and the
OPTIONS study (who started ART within 6 months after HIV diagnosis).
Participants underwent non-invasive assessment of arterial stiffness
using pulse wave analysis to determine the augmentation index and carotid-femoral
pulse wave velocity, a sensitive measure of cardiovascular risk.
Results
 |
In
unadjusted analyses, predictors of arterial stiffness included age,
blood pressure, diabetes, current CD4 T-cell count, and having nadir
CD4 count < 350 cells/mm3 (all P < 0.05). |
 |
After
adjusting for traditional cardiovascular risk factors (age, blood
pressure, diabetes, elevated cholesterol, smoking) and HIV status,
only having a lowest-ever CD4 cell count < 350 -- that is, below
the treatment threshold -- was independently associated with increased
pulse wave velocity and augmentation index. |
 |
Neither
ART use overall nor exposure to protease inhibitors was associated
with greater arterial stiffness. |
"Among
treated HIV-infected individuals, both traditional cardiovascular risk
factors as well as a low nadir CD4+ T-cell counts are associated with
arterial stiffness as assessed by augmentation index and pulse wave
velocity," the investigators concluded. "Our data suggest
that cardiovascular risk among HIV-infected individuals could be reduced
through early initiation of antiretroviral therapy, before CD4+ T-cell
counts are depressed."
Studies
125, 707, and 708: University of California at San Francisco and San
Francisco General Hospital, San Francisco, CA.
Study
709: Albert Einstein College of Medicine, Bronx, NY; University of California,
San Francisco, CA; Rush University Medical Center, Chicago, IL; Johns
Hopkins University, Baltimore, MD; University of Southern California,
Los Angeles, CA.
Study
126: University of Minnesota, Hennepin County Med Ctr, Minneapolis,
MN; CDC, Atlanta, GA; Univ of Southern California, Los Angeles, CA;
Washington Univ, St Louis, MO; Los Angeles Biomed Res Inst at Harbor-UCLA,
Torrance, CA.
3/12/10
References
P Hsue,
P Hunt, A Schnell, and others. Rapid Progression of Atherosclerosis
at the Carotid Bifurcation Is Linked to Inflammation in HIV-infected
Patients. 17th Conference on Retroviruses & Opportunistic Infections
(CROI 2010). San Francisco. February 16-19, 2010. Abstract 125.
P Hsue,
P Hunt, A Schnell, and others. Inflammation Is Associated with Endothelial
Dysfunction among Individuals with Treated and Suppressed HIV Infection.
17th Conference on Retroviruses & Opportunistic Infections (CROI
2010). San Francisco. February 16-19, 2010. Abstract 708.
R Kaplan,
E Sinclair, A Landay, and others. T Cell Senescence and T Cell Activation
Predict Carotid Atherosclerosis in HIV-infected Women. 17th Conference
on Retroviruses & Opportunistic Infections (CROI 2010). San Francisco.
February 16-19, 2010. (Abstract
709).
J Baker,
K Henry, P Patel, and others (CDC Study Investigators). Progression
of Carotid Intima-media Thickness in a Contemporary HIV Cohort. 17th
Conference on Retroviruses & Opportunistic Infections (CROI 2010).
San Francisco. February 16-19, 2010. Abstract 126.
J Ho,
S Deeks, F Hecht, and others. Earlier Initiation of ART in HIV-infected
Individuals Is Associated with Reduced Arterial Stiffness. 17th Conference
on Retroviruses & Opportunistic Infections (CROI 2010). San Francisco.
February 16-19, 2010. Abstract 707.