Research
Sheds New Light on HIV in the Gut
 |
 |
 |
 |
 |
 |
 |
| SUMMARY:
Different forms of HIV genetic material are concentrated in
different parts of the gastrointestinal tract, and HIV behavior
and immune response appears different in the gut than in the
blood, according to a poster presentation at the 17th Conference
on Retroviruses & Opportunistic Infections (CROI
2010) this week in San Francisco. |
|
 |
 |
 |
 |
 |
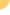 |
 |
By
Liz Highleyman
From the
earliest stages of infection, HIV causes injury to the lining of the
intestines as it infects the many CD4 T-cells present. This damage can
allow microbes residing in the gut to leak out. As these bacteria and
their toxins such as lipopolysaccharide (LPS) enter the bloodstream
a process known as microbial translocation they trigger systemic immune
activation, and the resulting inflammatory response appears to contribute
to a variety of non-AIDS conditions seen in people
with HIV.
Steven Yukl and colleagues with the PLUS Study Group measured levels
of HIV RNA, DNA, and T-cell activation throughout the gut and in peripheral
blood mononuclear cells (immune cells such as lymphocytes, monocytes,
and macrophages).
"The gut is a major reservoir for HIV persistence in patients receiving
antiretroviral therapy
(ART)," they hypothesized. "Distinct immune environments
within the gut may support varying levels of HIV."
The study
included 8 HIV positive patients on ART with a CD4 cell count > 200
cells/mm3 and plasma HIV RNA < 40 copies/mL for 3 to 12 years. The
researchers obtained blood plasma, peripheral blood mononuclear cells,
and endoscopic biopsies taken from the duodenum, terminal ileum, right
colon, and rectum (different parts of the large and small intestine).
T-cell subsets and activation markers (CD38, HLA-DR) were measured in
peripheral cells and gut cells using flow cytometry.
Results
 |
Low-level
plasma HIV RNA was detectable in all patients using a highly sensitive
assay (median 2.3 copies/mL). |
 |
Unspliced
HIV RNA was detectable at each gut site in the majority of patients
(63% to 88%) using real time PCR, but was undetectable using in
situ hybridization. |
 |
HIV
DNA levels increased from the duodenum (the first section of the
small intestine) to the rectum (the last section of the large intestine). |
 |
HIV
DNA per CD4 T-cell was higher at all 4 gut sites compared with peripheral
blood mononuclear cells (ratios of 2.8 for duodenum, 6.5 for ileum,
6.3 for colon, and 9.1 for rectum). |
 |
The
median unspliced HIV RNA (copies per CD4 cell) was also higher at
all gut sites compared to peripheral blood mononuclear cells, peaking
in the ileum (ratio 10.2). |
 |
HIV
DNA correlated positively with T-cell activation markers in the
peripheral blood mononuclear cells, but negatively with T-cell activation
in the gut. |
 |
The
ratio of unspliced HIV RNA to HIV DNA (transcriptional activity
per infected cell) decreased from the small to the large intestine.
|
 |
Multiply
spliced RNA was detected infrequently in gut (0% to 16.7%) relative
to peripheral blood mononuclear cells (50%). |
 |
RNA/DNA
ratios were lower in the colon (median 0.01) and rectum (also 0.01)
relative to peripheral blood mononuclear cells (median 0.06), reflecting
" |
 |
paradoxically
low HIV transcription given the higher level of T-cell activation
in the gut. |
"HIV
DNA and RNA are both concentrated in the gut relative to blood, but
HIV RNA is highest in the ileum whereas HIV DNA is highest in the rectum,"
the researchers concluded. "The inverse relationship between HIV
DNA and T-cell activation in the gut and the paradoxically low levels
of HIV expression in the large bowel suggest that different processes
drive HIV persistence in the blood and gut."
San
Francisco VAMC and University of California, San Francisco, CA; University
Hospital Zurich, Switzerland; University of Minnesota, Minneapolis,
MN; San Francisco General Hospital and University of California, San
Francisco, CA.
2/26/10
Reference
S
Yukl, S Gianella, Q Li, and others (PLUS Study Group). Differences in
HIV Burden throughout the Gut of Patients on Suppressive ART: Implications
for HIV Persistence. 17th Conference on Retroviruses & Opportunistic
Infections (CROI 2010). San Francisco. February 16-19, 2010. Abstract
97.