Anal
Pap Smears to Detect Pre-cancerous Cell Changes Are as Effective
as Cervical Screening, especially at Low CD4 Counts
 |
 |
 |
 |
 |
 |
 |
| SUMMARY:
Anal cytology testing works about as well as cervical
cytology tests -- better known as Pap smears -- for
detecting pre-cancerous cell changes (neoplasia) in
HIV positive and HIV negative individuals, according
to a study published in the January
28, 2010 issue of AIDS. The test was more
accurate for higher grades of neoplasia, for HIV positive
participants, and for those with lower CD4 cell counts.
|
|
 |
 |
 |
 |
 |
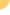 |
 |
By
Liz Highleyman
Several
studies have shown that people with
HIV are more likely to develop anal
cancer compared with the HIV negative general population,
and that the risk rises as CD4 count falls. Invasive cervical
cancer is classified as an AIDS-defining condition in HIV
positive women. However, anal cancer is not similarly designated,
even though it is caused by the same high-risk types of human
papillomavirus (HPV).
Pap
smear cytology testing involves collecting a sample of cells and
examining them under a microscope for unusual changes. Among women
in the general population, the widespread adoption of regular
Pap screening starting in the 1950s dramatically reduced the rate
of death due to cervical cancer.
HIV
positive women are more likely than negative women to be infected
with high-risk HPV types and to have pre-cancerous cell changes.
However, in industrialized countries, they do not have a higher
rate of cervical cancer death, which is attributed to regular
Pap screening to detect changes at an early, treatable stage.
Anal cytology screening is not currently considered part of the
standard of care for at-risk HIV positive people, but some experts
believe it should be.
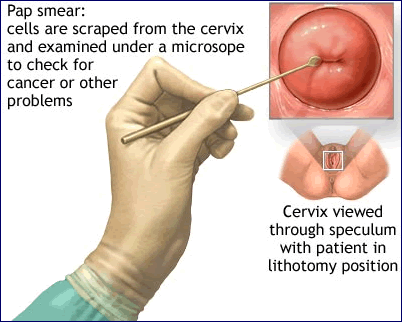
 In
the present study, Mayura Nathan from Homerton University Hospital
in London and colleagues assessed the performance of anal cytology
as a screening tool, comparing cytology testing versus histology
testing (using tissue biopsy specimens) and high-resolution anoscopy
(examination of the anal canal and rectum using a lighted magnifying
instrument).
In
the present study, Mayura Nathan from Homerton University Hospital
in London and colleagues assessed the performance of anal cytology
as a screening tool, comparing cytology testing versus histology
testing (using tissue biopsy specimens) and high-resolution anoscopy
(examination of the anal canal and rectum using a lighted magnifying
instrument).
The
study included a total of 395 participants (367 men and 28 women)
referred for follow-up examination due to suspected anal abnormalities.
Just over half (54%) were HIV positive and 39% were HIV negative.
About three-quarters were men who have sex with men (MSM), a group
at increased risk for anal cancer.
The researchers obtained an anal Pap test specimen prior to anoscopy
examination and tissue biopsy in the same individual, and evaluated
agreement between the methods. In total, they analyzed 584 cytology
specimens and 288 histology specimens.
They reported diagnostic accuracy in terms of sensitivity (number
of cases correctly identified), specificity (absence of pathology
correctly ruled out), and negative predictive value (proportion
of patients without pathology correctly diagnosed).
Results
 |
Measured
against histology results, the sensitivity of anal cytology
to detect any degree of disease was 70% and specificity was
67%. |
 |
For
high-grade disease including anal intraepithelial neoplasia,
the sensitivity of anal cytology was 81% and the negative
predictive value was 85%. |
 |
Sensitivity
depended on the extent of disease, and was more accurate if
there were cell changes in 2 or more quadrants (86%) compared
with 1 or more quadrants (69%). |
 |
Sensitivity
was higher for MSM (71%) compared with heterosexual participants
(59%). |
 |
Sensitivity
was higher for HIV positive participants (76%) than for HIV
negative people (59%). |
 |
Among
HIV positive individuals, the sensitivity was 90% when CD4
count was 400 cells/mm3 versus 67% when it was > 400 cells/mm3. |
Based
on these results, the study authors concluded, "Anal cytology
performs similar to cervical cytology in a clinical setting."
"Sensitivity of anal smear is dependent on the area (quadrants)
of disease present," they continued. "Sensitivity of
anal cytology is enhanced when CD4 cell count is less than 400
cells/[mm3] in HIV positive men."
They added that their findings might help explain the variable
sensitivity results observed in prior studies.
"Given the inaccuracies that exist with any method of evaluation,
we need to have a number of assessment methods for the diagnosis
of anal neoplasia, as is the case with cervical neoplasia,"
they recommended in their discussion. "This study supports
the introduction of earlier screening in HIV positive patients,
given their higher burden of anal disease and increased sensitivity
with lower CD4 cell count levels."
Department of Sexual Health, Homerton University Hospital NHS
Foundation Trust, London, UK.
1/26/10
References
M Nathan, N Singh, N Garrett, and others. Performance of anal
cytology in a clinical setting when measured against histology
and high-resolution anoscopy findings. AIDS 24(3): 373-379
(Abstract).
January 28, 2010.
L Pantanowitz and BJ Dezube. The anal Pap test as a screening
tool (Editorial comment). AIDS 24(3): 463-465. January
28, 2010.
