Opportunistic
Infections in the U.S. during the Combination Antiretroviral Therapy
Era
 |
 |
 |
 |
 |
 |
 |
| SUMMARY:
The
incidence of opportunistic infections and cancers declined
steeply after the introduction of effective combination
antiretroviral therapy (ART) in the mid-1990s and then
reached a plateau during the mid-2000s, according to
an analysis of the large HOPS cohort reported in the
June
19, 2010 issue of AIDS. More than one-third
of people who developed opportunistic illnesses, however,
did so at CD4 cell counts of 200 cells/mm3 or higher.
|
|
 |
 |
 |
 |
 |
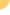 |
 |
By
Liz Highleyman
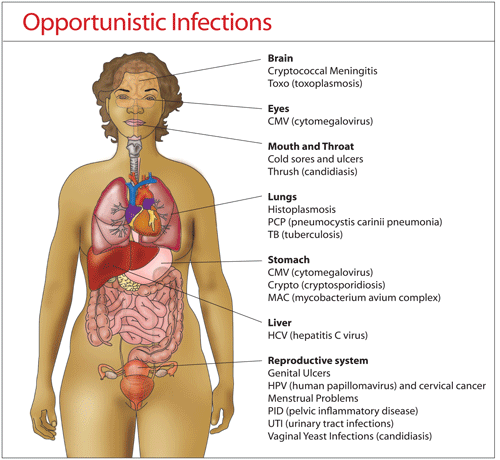
The widespread introduction of multi-class
combination antiretroviral regimens starting in the mid-1990s
dramatically reduced the incidence of and mortality related to
opportunistic illnesses (OIs),
or infections and malignancies that occur when the immune system
is severely compromised.
But a significant proportion of people
with HIV in North America and Europe do not get tested and
diagnosed until they already have advanced disease -- and too
many people in developing countries still do not have access to
state-of-the-art treatment -- so OIs remain a concern.
Kate
Buchacz and fellow investigators with the HIV Outpatient Study
(HOPS) performed an analysis of AIDS-defining opportunistic illness
rates, types, and risk factors in this large cohort -- one of
only a few major OI studies reported in recent years.
This
prospective cohort study included 8070 HIV positive HOPS participants
seen at 12 U.S. HIV clinics. A majority were men, people of diverse
race/ethnicity were included, and the median age at baseline was
38 years. The median CD4 cell count was 298 cells/mm3 -- below
the U.S.
treatment guidelines threshold for initiating antiretroviral
treatment.
The researchers calculated incidence (new case) rates per 1000
person-years of follow-up for the first opportunistic infection,
first opportunistic malignancy, and first occurrence of each specific
OI between 1994 -- just prior to the advent of combination ART
-- and 2007. The 3 AIDS-defining cancers are Kaposi's sarcoma
(KS), non-Hodgkin lymphoma (NHL), and cervical cancer; anal cancer
is not classified as an OI even though it is caused by the same
high-risk human papillomavirus strains. They then modeled annual
percentage changes in OI incidence rates by calendar period, adjusting
for sex, race/ethnicity, and HIV risk category.
Results
 |
The
8070 participants collectively developed 2027 new opportunistic
illnesses during a median 3 years of follow-up per person. |
 |
Opportunistic
infection rates fell steeply soon after the introduction of
ART, then showed a slower decline: |
| |
 |
1994-1997:
89.0 cases per 1000 person-years; |
 |
1998-2002:
25.2 cases per 1000 person-years; |
 |
2003-2007:
13.3 cases per 1000 person-years. |
|
 |
A
similar pattern was observed for opportunistic malignancies,
though numbers were smaller: |
| |
 |
1994-1997:
23.4 cases per 1000 person-years; |
 |
1998-2002:
5.8 cases per 1000 person-years; |
 |
2003-2007:
3.0 cases per 1000 person-years. |
|
 |
Decreases
in opportunistic illness rates were similar when looking only
at the subset of patients receiving combination ART -- a proportion
that rose over time. |
 |
During
2003-2007, there were no significant changes in annual rates
of opportunistic infections or malignancies. |
 |
"
The most common opportunistic illnesses were as follows: |
 |
 |
Esophageal
candidiasis or thrush: 5.2 cases per 1000 person-years; |
 |
Pneumocystis
pneumonia (PCP): 3.9 per 1000 person-years; |
 |
Cervical
cancer: 3.5 per 1000 person-years; |
 |
Mycobacterium
avium complex (MAC): 2.5 per 1000 person-years; |
 |
Cytomegalovirus
(CMV) disease: 1.8 per 1000 person-years. |
|
 |
36% of opportunistic illnesses occurred at a CD4 cell count
of 200 cells/mm3 or higher. |
Based
on these findings, the study authors concluded, "Opportunistic
illness rates declined precipitously after introduction of combination
ART and stabilized at low levels during 2003-2007."
In the contemporary combination ART era, they continued, "a
third of opportunistic illnesses were diagnosed at CD4 cell counts
at least 200 cells/[mm3]" -- the threshold for an AIDS diagnosis
and the level usually considered to mark the OI danger zone where
prophylaxis therapies should be considered.
Investigator
affiliation: Divisions of HIV/AIDS Prevention, National Center
for HIV, Hepatitis, STD, and TB Prevention, Centers for Disease
Control and Prevention, Atlanta, GA.
8/31/10
Reference
K
Buchacz, RK Baker, FJ Palella, and others (HOPS Investigators).
AIDS-Defining Opportunistic Illnesses in U.S. Patients, 1994-2007:
A Cohort Study. AIDS 24(10): 1549-1559 (Abstract).
June 19, 2010.
