People
with HIV Have Good Kidney Transplant Outcomes
 |
 |
 |
 |
 |
 |
 |
| SUMMARY:
HIV positive people can safely undergo kidney transplantation
and achieve survival outcomes nearly as good as
those of HIV negative individuals, according to
research published in the November
18, 2010 New England Journal of Medicine.
Nearly 90% of HIV positive kidney recipients were
still alive 3 years after transplantation, with
no increase in HIV-related complications, but this
group did have a higher than expected rate of organ
rejection. |
|
 |
 |
 |
 |
 |
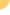 |
 |
By
Liz Highleyman
Early
in the AIDS epidemic, most clinicians considered people
with HIV to be poor candidates for organ transplants,
due to comprised immune function and limited life expectancy.
Since the advent of effective combination
antiretroviral therapy (ART) in the mid-1990s, though,
a growing number of centers now perform transplants for this
population.
Peter
Stock and Michele Roland from the University of California
at San Francisco and colleagues conducted a prospective, non-randomized
trial of kidney transplantation in HIV positive patients with
undetectable viral load on ART and CD4 T-cell counts of at
least 200 cells/mm3.
The
ability of people with HIV to undergo kidney transplantation
is important because end-stage renal disease (ESRD) is relatively
common in this population, especially among black patients,
the study authors noted as background.
Between
November 2003 and June 2009, a total of 150 HIV positive patients
at 19 medical centers underwent kidney transplantation. Most
(78%) were men, the median age was 46 years, and 69% were
black. The median CD4 count at the time of transplantation
was 524 cells/mm3.
Participants were followed for a median of 1.7 years. Post-transplant
management was provided in accordance with study protocols
that included guidelines for prophylaxis against opportunistic
infections, indications for biopsy, use of immune-suppressing
medications to prevent organ rejection, and continued use
of ART.
Results
 |
1
year after transplantation, the patient survival rate
was 94.6%. |
 |
At 3 years, this rate remained high, at 88.2%. |
 |
Rates
of graft, or donor kidney, survival were 90.4% at 1 year
and 73.7% at 3 years. |
 |
However,
organ rejection occurred more often than expected, with
49 patients (33%) experiencing 67 acute rejection episodes. |
 |
Based
on this finding, the rejection rate was estimated at 31%
by 1 year and 41% by 3 years. |
 |
In
a multivariate analysis, patients treated for organ rejection
and those receiving anti-thymocyte globulin induction
therapy were significantly more likely to experience graft
loss (hazard ratios 2.8 and 2.5, respectively). |
 |
Patients
who received kidneys from living donors rather than cadavers
experienced significantly less graft loss (hazard ratio
0.2). |
 |
In
general, HIV infection remained well controlled, with
stable CD4 counts and few HIV-associated complications. |
 |
7
patients, however, progressed to AIDS (CD4 count <
200 cells/mm3 or AIDS-defining opportunistic illness). |
 |
Use
of anti-thymocyte globulin was linked to greater CD4 cell
loss. |
 |
57
patients (38%) experienced a total of 140 reported infections
that required hospitalization (69% bacterial, 9% fungal,
6% viral, and 1% protozoal). |
"In
this cohort of carefully selected HIV-infected patients, both
patient- and graft-survival rates were high at 1 and 3 years,
with no increases in complications associated with HIV infection,"
the study authors concluded.
They
noted that, in general, patient and graft survival rates in
this study were a bit lower than rates reported in the national
transplant database for all kidney transplant recipients,
but higher than those for transplant recipients age 65 or
older.
But
the rate of kidney rejection in this study was about 2 to
3 times higher than usual. Even though early organ rejection
could often be managed, thus saving the kidney, the researchers
said, "The unexpectedly high rejection rates are of serious
concern and indicate the need for better immunotherapy."
In an accompanying editorial, Lynda Szczech from Duke University
Medical Center wrote that, "Stock and his colleagues
have now challenged assumptions that seemed intuitive but
were unsupported and have shown that transplantation may greatly
improve the lives of patients with HIV and ESRD. The next
step is to develop effective treatments for all HIV-related
kidney diseases before they progress to ESRD."
Investigator affiliations: University of California at
San Francisco, San Francisco, CA; EMMES Corporation, Rockville,
MD; Mount Sinai School of Medicine, New York, NY; Beth Israel
Deaconess Medical Center, Boston, MA; University of Miami
School of Medicine, Miami, FL; Washington Hospital Center,
Washington, DC; Georgetown University, Washington, DC; University
of Maryland, Baltimore, MD; Johns Hopkins University School
of Medicine, Baltimore, MD; University of Pennsylvania, Philadelphia,
PA; Drexel University College of Medicine, Philadelphia, PA;
Rush University Medical Center, Chicago, IL; University of
Chicago, Chicago, IL; Northwestern University, Chicago, IL;
Emory University, Atlanta, GA; University of Virginia, Charlottesville,
VA; Tulane Medical Center, New Orleans, LA; University of
Pittsburgh, Pittsburgh, PA.
12/3/10
References
PG
Stock, B Barin, B Murphy, M Roland, and others. Outcomes of
kidney transplantation in HIV-infected recipients. New
England Journal of Medicine 363(21): 2004-2014 (Abstract).
November 18, 2010.
LA
Szczech. Tackling the unknowns in HIV-related kidney diseases
(Editorial). New England Journal of Medicine 363(21):
2058-2059. November 18, 2010.
