Inflammation
Linked to Higher Mortality Even for People with High CD4 Cell
Counts
 |
 |
 |
 |
| SUMMARY:
Inflammation was associated with an increased risk
of death among HIV positive participants in the
FRAM study, according to a report in the November
1, 2010 Journal of Acquired Immune Deficiency
Syndromes Inflammation. People with the
highest levels of 2 inflammation biomarkers -- fibrinogen
and CRP -- had more than 2.5-fold higher mortality
than those with the lowest levels. Inflammation
remained a predictor of mortality even among people
with CD4 counts above 500 cells/mm3. |
|
 |
 |
 |
 |
By
Liz Highleyman
A growing body of evidence suggests that chronic inflammation
triggered by persistent virus may help explain the higher
rates of cardiovascular disease, neurocognitive dysfunction,
and other chronic conditions seen in people with HIV
-- even those with high CD4 T-cell counts and well-preserved
immune function.
To
further explore this issue, Phyllis Tien, Carl Grunfeld, and
fellow investigators with the FRAM (Fat Redistribution and
Metabolic Change in HIV Infection) study looked at the association
between levels of 2 inflammatory markers, fibrinogen and C-reactive
protein (CRP), and 5-year mortality risk.
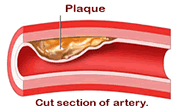 Fibrinogen
and CRP are acute-phase proteins released as part of the inflammation
and clotting cascade that occurs with development of atherosclerosis,
or blood vessel narrowing that can lead to heart attack or
stroke.
Fibrinogen
and CRP are acute-phase proteins released as part of the inflammation
and clotting cascade that occurs with development of atherosclerosis,
or blood vessel narrowing that can lead to heart attack or
stroke.
The
analysis included 922 HIV positive FRAM participants. A majority
(about 70%) were men, the median age was 42 years, and 40%
were current smokers. Most (about 90%) had used antiretroviral
therapy (ART), about 80% had undetectable viral load,
and the average CD4 cell count was about 350 cells/mm3. Participants
were followed for 5 years.
Results
 |
Participants with fibrinogen levels in the highest tertile
or third (> 406 mg/dL) had a 2.6-fold higher risk of
death than people with levels in the lowest tertile (<
319 mg/dL). |
 |
Participants
with high CRP (> 3 mg/L) had a 2.7-fold higher risk
of death than those with CRP < 1 mg/L. |
 |
When
stratified according to CD4 count, fibrinogen remained
independently associated with increased mortality, with
the greatest effect seen among people with the lowest
counts: |
| |
 |
<
200 cells/mm3: odds ratio 1.93, or nearly twice
the risk of death; |
 |
200-350
cells/mm3: odds ratio 1.43; |
 |
351
to 500 cells/mm3: odds ratio 1.43; |
 |
>
500 cells/mm3: odds ratio 1.30. |
|
 |
Higher
CRP remained associated with higher risk of death overall
and within each CD4 count subgroup. |
Based
on these findings, the study authors concluded, "Fibrinogen
and CRP are strong and independent predictors of mortality
in HIV-infected adults."
"Our
findings suggest that even in those with relatively preserved
CD4 counts > 500 [cells/mm3], inflammation remains an important
risk factor for mortality," they continued. "Further
investigation should determine whether interventions
to reduce inflammation might decrease mortality risk in
HIV-infected individuals."
The
researchers noted in their discussion that these findings
support the observations from the SMART
trial, which found that higher levels of the inflammation
biomarkers CRP, interleukin 6 (IL-6), and D-dimer were associated
with greater risk of death, progression to AIDS, and non-AIDS
conditions such as cardiovascular, kidney, and liver disease.
"The
strength of our study was the wide spectrum of CD4 levels
in our participants, which allowed us to examine the effect
of immunosuppression severity on the association of inflammation
with mortality," they wrote. "As expected, we found
that the [odds ratio] for mortality associated with fibrinogen
and CRP was greatest in magnitude for those with CD4 <
200. However, more important is our finding that higher fibrinogen
and CRP levels remained associated with increased mortality
risk in participants with CD4 > 500."
Investigator
affiliations: Department of Medicine, University of California,
San Francisco, San Francisco, CA; Department of Medicine,
San Francisco Veterans Affairs Medical Center, San Francisco,
CA; Department of Medicine, Stanford University, Stanford,
CA; Department of Medicine, University of California, San
Diego, San Diego, CA; |Department of Pathology and Biochemistry,
University of Vermont, Colchester, VT; Department of Epidemiology
and Biostatistics, University of California, San Francisco,
CA.
2/25/11
Reference
PC
Tien, AI Choi, AR Zolopa, C Grunfeld, and others. Inflammation
and Mortality in HIV-infected Adults: Analysis of the FRAM
Study Cohort. Journal of Acquired Immune Deficiency Syndromes
55(3): 316-322 (abstract).
November 1, 2010.
