HIV
Coreceptor Tropism Affects Treatment Outcomes
SUMMARY
HIV strains that use the CXCR4 co-receptor are associated
with higher risk of virological failure on antiretroviral
therapy than those using CCR5, according to a recent Spanish
study. |
By
Liz Highleyman
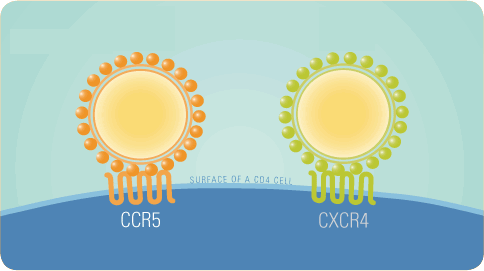
HIV uses 1 of 2 co-receptors -- CCR5 or CXCR4 -- along with
the CD4 receptor to enter cells. Prior research has shown
that virus using CXCR4 (known as CXCR4-tropic) is associated
with more advanced disease progression among untreated people,
but the effect of tropism on response to antiretroviral
therapy (ART) is not well understood.
|
Tropism
is the co-receptor HIV uses to get into your cells
|
 |
As
described in the July
2011 Journal of Infectious Diseases, Eduardo Seclén
from Hospital Carlos III in Madrid and colleagues compared
viral suppression according to co-receptor tropism in HIV
positive people starting ART for the first time.
The
analysis included 569 participants in the ArTEN trial, which
compared first-line boosted atazanavir
(Reyataz) versus nevirapine
(Viramune), both in combination with tenofovir/emtricitabine
(the drugs in Truvada).
A total of 428 patients completed 48 weeks of therapy, 146
in the atazanavir arm and 282 in the nevirapine group.
The
researchers retrospectively tested baseline plasma samples
collected prior to treatment initiation, using the "geno2pheno
FPR=5.75%" genotypic tool to determine tropism.
Results
 |
96
people (22%) had HIV-1 non-B subtypes, which are prevalent
outside Europe and the U.S. |
 |
55
patients (14%) had CXCR4-tropic virus prior to starting
treatment. |
 |
People
with CXCR4-tropic HIV had higher baseline plasma viral
load than those with CCR5-tropic virus (5.4 vs 5.2 log
copies/mL, respectively, a difference that just reached
statistical significance). |
 |
People
with CXCR4-tropic HIV also had significantly lower CD4
cell counts at baseline (145 vs 188 cells/?L, respectively).
|
 |
At
week 48 of treatment, the virological response rate was
significantly lower in people with CXCR4-tropic compared
with CCR5-tropic virus (77% vs 92%, respectively). |
 |
In
a multivariate analysis, HIV tropism was an independent
predictor of virological response overall at week 24. |
 |
Tropism
was also predictor of virological response at week 48
in people with clade B virus subtypes. |
 |
Baseline
co-receptor tropism was not, however, significantly associated
with immunological response, or CD4 cell count recovery.
|
Based
on these findings, the study authors concluded, "HIV-1
tropism is an independent predictor of virologic response
to first-line antiretroviral therapy. In contrast, it does
not seem to influence CD4 cell count recovery."
"[T]his observation may have important clinical implications
for the monitoring of antiretroviral therapy and interpretation
of comparative trials," they suggested.
Investigator affiliations: Department of Infectious Diseases,
Hospital Carlos III, Madrid, Spain; Boehringer Ingelheim,
Germany.
6/28/11
Reference
E
Seclén, V Soriano, MM González, et al. Impact
of Baseline HIV-1 Tropism on Viral Response and CD4 Cell Count
Gains in HIV-Infected Patients Receiving First-line Antiretroviral
Therapy. Journal of Infectious Diseases 204(1):139-144
(abstract).
July 2011.
