HIV
Infection Linked to Increased Cardiovascular Risk Even in Long-term Non-progressors
 |
 |
 |
 |
 |
|
| SUMMARY:
Markers of endothelial dysfunction -- an early indicator of
cardiovascular disease -- were elevated in HIV
positive people who maintained a stable viral load and
CD4 cell count without antiretroviral
therapy (ART), and even among "elite controllers,"
according to a study presented at the 50th Interscience Conference
on Antimicrobial Agents and Chemotherapy (ICAAC
2010) this week in Boston. This finding adds further evidence
that factors other than waning CD4 T-cell function -- for
example, persistent inflammation -- contribute to non-AIDS
conditions in the ART era. |
|
|
 |
 |
 |
 |
By
Liz Highleyman
Several
studies have shown that people with HIV have a higher rate of cardiovascular
disease and associated events compared with the HIV negative general
population, but it is not yet clear whether this is due to HIV infection
itself, antiretroviral therapy, traditional risk factors, or some combination
thereof.
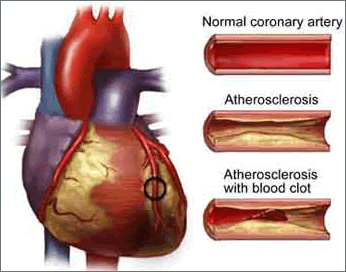 As
atherosclerosis progresses, arteries lose their elasticity, or ability
to expand, as they become filled with plaques. Eventually the blockage
can impair blood flow, and pieces of plaque or blood clots can break
away and become lodged in vessels supplying the heart (causing a heart
attack) or the brain (causing a stroke).
As
atherosclerosis progresses, arteries lose their elasticity, or ability
to expand, as they become filled with plaques. Eventually the blockage
can impair blood flow, and pieces of plaque or blood clots can break
away and become lodged in vessels supplying the heart (causing a heart
attack) or the brain (causing a stroke).
Atherosclerosis is an inflammatory process, and past research -- including
the large SMART
treatment interruption study -- has shown that people with HIV,
especially those with uncontrolled virus, have higher levels of biomarkers
(substances in the blood) associated with inflammation, coagulation
(clotting), and damage to the endothelial lining of blood vessels. In
addition, studies have shown that people with HIV are more likely to
show thickening
of the lining of the carotid arteries serving the brain (carotid
intima-media thickness, or IMT), and that this is also linked to inflammation.
At ICAAC, Hector Bonilla from Summa Health System in Akron and colleagues
presented a poster reporting findings from a cross-sectional case-control
study of early cardiovascular disease as measured by carotid IMT and
inflammation markers in long-term non-progressors (LTNPs), defined as
people who were HIV positive for at least 5 years and able to maintain
stable viral load and CD4 cell counts with no AIDS-defining illnesses
in the absence of ART.
The study
included 13 HIV positive LTNPs and 13 HIV negative control subjects
matched by age, sex, and race; 4 of the non-progressors were "elite
controllers," meaning they maintained long-term undetectable viral
load without treatment.
In the
HIV positive group, 9 participants were men, 7 were white, and 6 were
black. The mean age was 44 years, and they had been living with HIV
for an average of 13.5 years (range 5-24 years). They had relatively
early HIV disease on average, with a mean current CD4 count of 440 cells/mm3
(all above 325) and a mean nadir or lowest-ever CD4 count of 380 cells/mm3
(all 300 or higher).
Traditional
risk factors for cardiovascular disease were common, including smoking
(more than half of both groups, but higher in the HIV negative group),
abnormal blood lipids (more prevalent in the HIV positive group), and
being overweight.
The researchers
measured inflammation biomarkers including C-reactive protein (CRP),
soluble tumor necrosis factor receptor type 2 (sTNF-RII), soluble vascular
adhesion molecule (sVCAM), and adiponectin (a hormone produced by fat
tissue). Carotid IMT was assessed using B-mode ultrasound.
Results
 |
Overall,
carotid IMT was not significantly greater for HIV positive LTNPs
compared with HIV negative control subjects. |
 |
However,
when measured at the carotid bulb -- where the artery bifurcates
or forks and blood flow is turbulent -- there was a nearly significant
trend toward greater thickening among the LTNPs. |
 |
HIV
positive participants had higher sTNF-RII compared with the HIV
negative group -- the only biomarker than was significantly different
according to HIV status (P = 0.002). |
 |
Among
the LTNPs, elevated sVCAM1 showed a trend toward correlation with
greater carotid IMT (P = 0.014). |
 |
LTNPs
had lower high-density lipoprotein (HDL), or protective "good"
cholesterol, compared with the HIV negative group. |
 |
8
of 13 LTNPs had HDL < 40 mg/dL, the threshold for men considered
to indicate greater cardiovascular risk. |
"Endothelial
markers are significantly elevated in long-term non-progressors compared
to healthy controls, and correlate with carotid IMT measurements,"
the researchers concluded. "This emphasizes the effect of HIV itself
vs. ART" on heightened cardiovascular disease risk in people with
HIV.
In chronically
infected, untreated HIV positive patients, they added in an ICAAC media
advisory, "the persistent low grade viremia, the low levels of
HDL-C ("good cholesterol"), [and] the increased levels of
inflammation indicated by high levels of sTNF-RII, correlated with accelerated
atherosclerosis."
Investigator affiliations: Summa Hlth.System, Akron, OH; NEOUCOM,
Rootstown, OH; Case Western Reserve Cleveland, Cleveland, OH.
9/17/10
Reference
H Bonilla; J McShannic, D Chua, G. McComsey, and others. Cardiovascular
Disease (CVD) and Inflammatory Markers in Long Term Non-Progressors
(LTNP). 50th Interscience Conference on Antimicrobial Agents and Chemotherapy
(ICAAC 2010). Boston, September 12-15, 2010. Abstract
H-220.
Other
Source
ICAAC.
What is causing cardiovascular changes in HIV infected patients? Media
advisory. September 12, 2010.