By
Liz Highleyman
Recent
studies have produced conflicting data regarding the effect
of abacavir on cardiovascular outcomes. The
large D:A:D study and the SMART
treatment interruption trial showed that patients currently
taking abacavir-containing regimens were more likely to
experience heart attacks and other cardiovascular events.
However,
a meta-analysis
of more than 50 studies conducted by abacavir manufacturer
GlaxoSmithKline did not find such an association, and more
recent research suggests that confounding factors such
as kidney disease may explain the link.
The
mechanism by which abacavir might contribute to heart problems
is unclear, since it does not cause the type of blood lipid
abnormalities associated with some other antiretroviral
drugs. But, according to the new report in AIDS,
it may have an effect on blood vessel function.
Priscilla
Hsue from the Positive Health Program at San Francisco General
Hospital and colleagues tested the hypothesis that current
treatment with abacavir is associated with impaired endothelial
function.
The
study looked at a cohort of 61 HIV patients on stable antiretroviral
therapy (ART) for at least 6 months who had undetectable
plasma viral load. Most (95%) were men, the median age was
50 years, the median duration of HIV infection was 18 years,
and the median CD4 count was 369 cells/mm3. About half the
patients (n = 30) were taking abacavir.
Endothelial
function was assessed using flow-mediated dilation (FMD)
of the brachial artery in the upper arm, a measure of how
well blood vessels respond to changes in blood flow. The
investigators compared FMD in patients treated with or without
abacavir, adjusting for traditional risk factors (e.g.,
older age, high blood pressure, smoking) and HIV-related
characteristics.
Results
 |
Overall,
median FMD in the HIV positive patients regardless of
type of ART was low (3.5%), indicating impaired blood
vessel function and poorer blood flow. |
 |
FMD
was significantly lower, however, in the current abacavir-treated
group compared with patients not taking abacavir (2.8%
vs 4.9%; P = 0.01). |
 |
Among
5 patients who had taken abacavir in the past, FMD was
also lower compared to those with no prior history of
abacavir use (P = 0.04). |
 |
After
adjusting for traditional risk factors, HIV-specific
factors, and baseline brachial artery diameter, current
abacavir use remained independently associated with
lower FMD (P = 0.017). |
 |
Duration
of ART and CD4 count were not associated with reduced
FMD. |
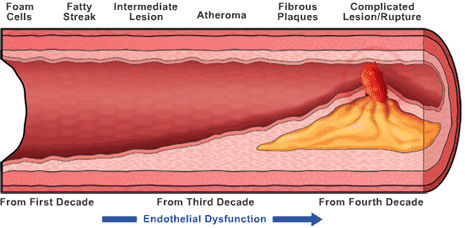
Based
on these findings, the study authors concluded, "Endothelial
function, a central mechanism in atherosclerosis and a marker
of cardiovascular risk, is impaired among antiretroviral-treated
patients with undetectable viral loads."
"Current
use of abacavir was independently associated with impaired
endothelial function," they continued. "This finding
suggests that abnormal endothelial function may underlie
the clinically observed increased risk in myocardial infarction
among abacavir-treated patients."
Further
research is needed to confirm these findings in a larger
patient population, and to shed light on the mechanisms
by which abacavir might impair blood vessel function. A
growing body of research indicates that chronic inflammation
contributes to non-AIDS illnesses such as heart disease
in people with HIV. Studies have produced mixed data, however,
about whether abacavir is associated with changes in markers
of inflammation.
Division
of Cardiology, Positive Health Program of the Department
of Medicine, San Francisco General Hospital, University
of California at San Francisco, San Francisco, CA.
10/23/09
Reference
P Hsue, PW Hunt, Y Wu, and others. Association of abacavir
and impaired endothelial function in treated and suppressed
HIV-infected patients. AIDS 23(15): 2021-2027. September
24, 2009. (Abstract).